Designing Mental Health Support for Healthcare Providers
All Ears | 2023 | 5 weeks -> Extended solo
MY ROLE
User Research | Insight Extraction | Concept Design | User Flow Mapping | UI Design | Prototyping | Iteration and Validation
TOOLS
Figma | FigJam | Adobe Illustrator | Miro
TEAM
Solo Project (originally 3-person group project, continued independently after first iteration)
![AdobeStock_315445482 [Converted].png](https://static.wixstatic.com/media/e2be9b_8162e77c976547278ab1b0809629fd0a~mv2.png/v1/crop/x_657,y_450,w_4338,h_2901/fill/w_693,h_464,al_c,q_85,usm_0.66_1.00_0.01,enc_avif,quality_auto/AdobeStock_315445482%20%5BConverted%5D.png)
Overview
The Challenge
Healthcare workers face unprecedented mental health crises - 62.8% of physicians reported burnout symptoms during the pandemic peak, yet 18% couldn't acess mental health services due to constraints, stigma, or cost barriers. Existing solutions were either office-based (requiring time healthcare workers don't have) or generic wellness apps (missing the unique pressures of healthcare environment).
The core problem wasn't just access, it was dignity. Healthcare workers needed support that respected their privacy, understood their specific pressures, and integrated seamlessly into their demanding workflows.
The Opportunity
Our class project aimed to design a mental health solution specifically for healthcare professionals. When the group dissolved after our submission, I saw an opportunity to dig deeper into the research insights and design a solution that truly addressed the dignity gap we'd uncovered.
Physician Burnout
Mental Health Access Gap
Peak Crisis
62.8%
of physicians reported at least one symptom of burnout during the 2021 pandemic peak - the highest rate ever recorded
Unmet Needs
18%
of healthcare workers needed mental health services but couldn't access them due to time constraints, stigma, or cost barriers
Workforce Impact
50%
of healthcare workers reported considering leaving their field due to pandemic-related mental health burden
Healthcare providers were facing mental health issues
What I inherited from the group research
Our team had conducted interviews with doctors and interns from Mass General, Boston, who shared their experiences of:
-
Constant pressure and long hours draining mental reserves
-
Emotional situations making it hard to maintain composure
-
Feeling like seeking help would signal weakness
-
No private space to decompress during shifts
-
Fear of judgement from supervisors if they were seen 'struggling'
What I discovered through deep analysis
After the group project ended, I revisited all our research artifacts and realized we'd been solving the wrong problem. The issue wasn't jsut making support accessible, it was about preserving dignity while doing so.
I mapped out the complete ecosystem of healthcare worker mental health:
-
When burnout trigger happens (post trauma, during back-to-back cases, after patient deaths)
-
Where support was needed (during shifts, not just after hours)
-
Who was most affected (residents, nurses, especially juniors)
-
Why existing solutions failed (visibility, time, stigma, lack of healthcare-specific understanding)
This led me to identify a critical point: privacy and confidentiality were prerequisites for adoption.

We identified 3 major barriers
Privacy Issues
Our first iteration, the physical wellness stations situated in hallways and receptions, completely failed because they made healthcare workers more visible and vulnerable while seeking help.
There is a fine line between normalizing seeking help and upholding the privacy that people require to feel comfortable being vulnerable.

Urgency Barrier
Healthcare workers need support during their shifts, not scheduled weeks out. Traditional therapy methods requiring appointments couldn't address acute stress moments.
The solution needed to work in sync with their work environment and be accessible within their workflow, rather than as separate scheduled events.
Generic Solutions
Existing wellness apps didn't understand healthcare specific trauma - patient deaths, medical errors, life-or-death decisions, compassion fatigue, etc.
Healthcare workers needed support that validated their unique experiences and provided resources tailored to medical professionals
Healthcare workers needed a privacy-first platform
After our wellness station failed, I redesigned the entire approach from a physical intervention to a privacy-first digital platform. The key goal was to meet healthcare workers where they are, with a solution that feels like a work tool, not a public admission of struggle.
I restructured the IA
I restructured the entire information architecture from scratch, creating:
-
Immediate access through existing SSO systems (Workday/staff portals)
-
Private dashboard accessible on personal or work devices
-
Contextual support tailored to healthcare-specific stressors
-
Flexible engagement - use during breaks, between patients, or at home
-
Professional resources - both peer support and licensed therapists familiar with healthcare
-
Normalizing accessing mental health support through integration with workflow

Dashboard Home
Dashboard decision: Progressive disclosure keeps the interface calm and scannable, making sure there is no decision fatigue or information overload.
-
Quick mood check-in using one tap to log current state
-
Personalized activity recommended based on mood patterns and available time
-
Recent sessions at a glance provide easy access to continue therapy or self-care activities
Self-Care Tools Library
Design decision: Organized by how much time users have (5 min, 15 min, 30+ min) rather than by category, because healthcare workers think in terms of break lengths
-
Time based filtering removes extra decision time
-
Healthcare-specific grounding exercises for post-trauma, compassion fatigue, recover, even personal issues.

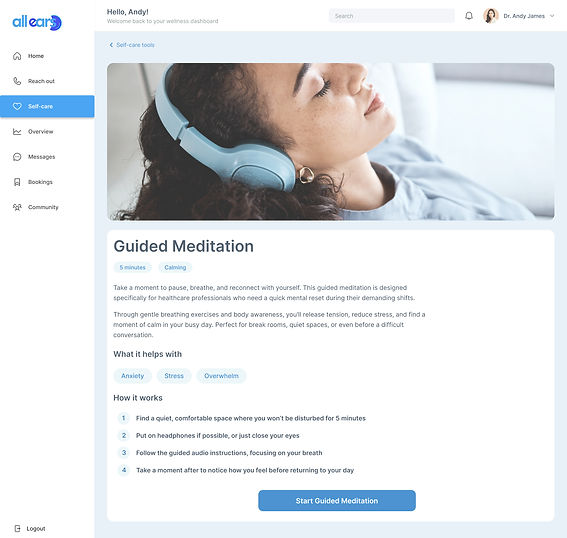
Activity Details
Design decision: Show exactly what to expect before starting - the duration, materials needed, what the activity involves, and how it helps
-
Clear expectation setting
-
Preview of Techniques
Therapist Booking
Design decision: Booking feels like any other professional service. Familiarity helps make it more natural
-
Therapist bio highlighting specializtions
-
Flexible schedules

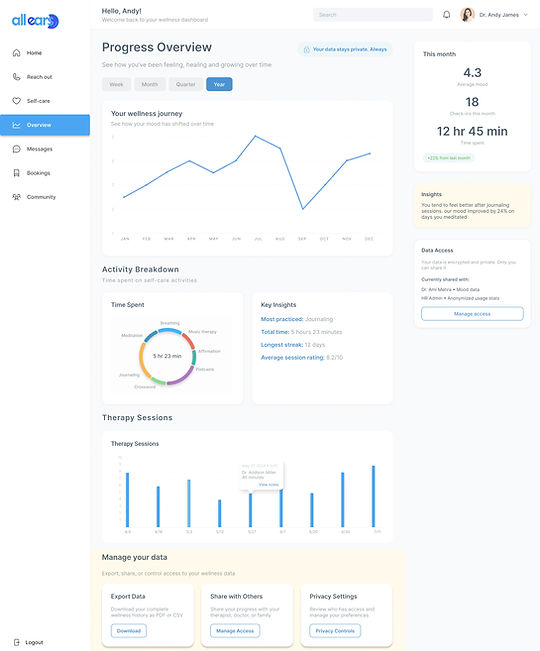
Progress Overview
Design decision: Visualize mental health journey as data while keeping it encouraging
-
Mood trends over time to spot patterns
-
Activity streaks to bring gamification
-
Correlation insights based on feedback
-
Sharing and privacy options to help users feel empowered and in control of their information
I validated the design
Since this was a class project that I extended independently, I validated the design through
Usability testing with 5 healthcare workers
-
100% said that they would use this over physical wellness stations
-
"I actually think my hospital should get something like this." - Trauma nurse
-
"Everyone says you get used to it. I haven't and this would make it so much easier."
Key behavior changes the design enables:
-
Reduces stigma by making mental health support integrated into existing workflows
-
Increases accessibility by meeting users where they are (through staff portals)
-
Normalizes mental health care by framing it as professional development, not personal weakness
Reflections
This project taught me that some problems aren't technical. Mental health support is very normalized in the world, however, it takes understanding, care, and integration to be useful in people's lives.
After we had submitted our project (we were on a very short timeline), I knew I wanted to work on it and bring it to fruition. Choosing to dig deeper forced me to
-
Own the design process from research analysis through final screens
-
Make strategic decisions about scope and prioritization
-
Trust my design instincts
-
Create a cohesive system across multiple touchpoints.
With more time, I would
-
Design the integration with existing hospital systems
-
Design the multi-sided platform like the therapist portal and administrator dashboard
-
Create mobile version
-
Develop a data privacy framework

